Breast health is a topic that concerns many, yet often remains shrouded in mystery. From the teenage years to post-menopause, understanding and maintaining breast health is crucial for every woman. In this guide, we’ll delve into proactive steps tailored for different age groups to ensure optimal breast health throughout life.
Teenage Years (13-19)
The teenage years are a transformative period, both emotionally and physically. One of the most significant changes for many young women is the onset of puberty, which brings about breast development. The development of breasts is primarily driven by hormonal changes, especially the increase in estrogen. This hormone signals the body to start creating breast tissue.

Variability is the Norm
It’s crucial for teenagers to understand that breast development is a highly individualized process. Some might notice growth as early as 8 or 9, while others might not see significant changes until their late teens. The size, shape, and even the rate at which breasts grow can vary widely. Some may develop quickly, while others might take years before they feel their breasts have “fully” grown.
No “Normal” Size or Shape
Society and media often portray an “ideal” when it comes to breast size and shape. However, there’s no universal standard for what breasts should look like. They can be large, small, round, teardrop-shaped, symmetrical, or asymmetrical. All these variations are entirely natural.
Statistics on Breast Cancer and Teenagers
Although breast cancer in teenagers is extremely rare, this does not mean that teens should not be proactively aware of the risks of not getting checked.
Here are some statistics on breast cancer and tennagers:
- American Cancer Society (ACS): According to the ACS, less than 5% of all breast cancers diagnosed in the U.S. occur in women under 40. While this statistic encompasses a broader age range than just teenagers, it underscores the rarity of breast cancer in younger women.
- Young Survival Coalition (YSC): The YSC notes that while breast cancer in young women accounts for a small percentage of all breast cancers, when it does occur, it tends to be more aggressive and has a lower survival rate. Again, this information is more relevant to young adults rather than teenagers specifically.
- BreastCancer.org: They state that while the overall risk of breast cancer for young women is low, certain genetic mutations (like BRCA1 and BRCA2) can increase the risk. However, even in these cases, the onset of breast cancer during teenage years is exceedingly rare.
20s and 30s
Breast health during the 20s and 30s is a crucial topic, as this is a time of significant life changes for many women, from career moves to pregnancies. While the risk of breast cancer remains relatively low compared to older age groups, it’s essential to be proactive about breast health during these years.
Understanding the Risk
When breast cancer does occur in younger women, it tends to be more aggressive. And women with a family history of breast cancer or those who carry mutations in the BRCA1 and BRCA2 genes have a higher risk. BreastCancer.org states that women with a BRCA1 mutation have a 55-65% chance of developing breast cancer by age 70, and those with a BRCA2 mutation have a 45% chance.

Proactive Steps for Breast Health in Your 20s and 30s
While the 20s and 30s are a time when the risk of breast cancer is lower, it’s a crucial period for establishing habits and routines that prioritize breast health. Regular check-ups, awareness of personal risk factors, and healthy lifestyle choices can set the foundation for lifelong breast health.
- Regular Self-Exams: While there’s debate about the effectiveness of breast self-exams in reducing mortality from breast cancer, they can still be a valuable tool for women to understand what’s normal for their bodies and to detect any changes. The ACS recommends that women become familiar with the typical look and feel of their breasts.
- Clinical Exams: Women in their 20s and 30s should have a clinical breast exam as part of their regular health check-ups, ideally every three years.
- Mammograms: Routine mammograms are generally not recommended for women under 40 unless they have specific risk factors. However, women with a high risk, such as those with BRCA mutations, might start screening earlier based on their doctor’s recommendations.
- Lifestyle Choices: Maintaining a healthy lifestyle can reduce the risk of breast cancer. This includes staying physically active, limiting alcohol intake, and avoiding smoking. The World Cancer Research Fund suggests that about 12% of breast cancers could be prevented through dietary and weight-related choices.
40s
The 40s are a pivotal decade for women’s breast health. As women age, the risk of breast cancer increases, making proactive measures even more crucial. Here’s a deeper dive into the importance of mammograms and the continued significance of self and clinical exams during this decade.
Mammograms in the 40s
Why Start in the 40s? The breast tissue tends to be denser in younger women, which can make mammograms less effective. However, by the 40s, the breast tissue often becomes less dense, making mammograms more effective in detecting abnormalities.
- Early Detection: One of the primary benefits of mammograms is their ability to detect tumors that might be too small to be felt. Early detection can lead to earlier intervention, which can significantly improve outcomes. According to the American Cancer Society (ACS), mammograms have been shown to reduce breast cancer mortality by 20-40% among women aged 40-74.
- Understanding the Process: A mammogram involves placing the breast between two plates, which then compress the breast to obtain clear X-ray images. While the compression can be uncomfortable, it’s brief. The entire procedure typically takes about 20 minutes.
- CDC’s Take on Mammograms: The Centers for Disease Control and Prevention (CDC) emphasizes the importance of mammograms as the best tool available for detecting breast cancer early. They provide resources and guidelines to help women make informed decisions about when and how often to get screened.
Continued Self and Clinical Exams
- Self-Exams: While the debate continues about the effectiveness of self-exams in reducing breast cancer mortality, they remain a valuable tool for many women. Regular self-exams help women stay familiar with their breasts, making it easier to notice any changes.
- Clinical Exams: A clinical breast exam is performed by a healthcare professional who checks the breasts and underarm for any lumps or changes. The ACS recommends that women in their 40s have a clinical breast exam as part of their regular health routine, ideally annually.
- The Synergy of Both: While mammograms are crucial, combining them with regular self-exams and clinical exams provides a comprehensive approach to breast health. Each method can detect changes that the others might miss.
50s and Beyond
As women transition into their 50s and beyond, their bodies undergo significant changes, many of which are influenced by hormonal shifts associated with menopause. These changes not only affect breast health but also have implications for overall well-being. Here’s a more in-depth exploration of the key aspects of breast health and related concerns for women in this age group.
Regular Mammograms
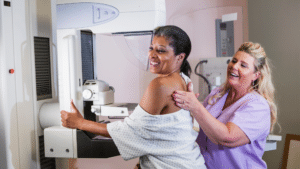
- The Continued Importance: The risk of breast cancer increases with age. According to the ACS, the median age of diagnosis for breast cancer in women in the U.S. is 62. This underscores the importance of regular mammograms as women age.
- Frequency of Mammograms: While women in their 40s are often advised to have annual mammograms, the recommendation for women in their 50s can vary. Some guidelines suggest every one to two years, but the exact frequency should be based on individual risk factors, previous mammogram results, and discussions with healthcare professionals.
- Advanced Screening Options: As technology advances, there are now more sophisticated mammogram options, such as 3D mammography (tomosynthesis), which can provide clearer images and detect abnormalities with greater accuracy, especially in women with dense breast tissue.
Post-Menopausal Changes
- Hormonal Shifts: Menopause marks the end of a woman’s reproductive years, characterized by the cessation of menstrual periods. This transition is accompanied by a decline in estrogen levels, which can lead to various changes in the breasts.
- Breast Composition: Post-menopause, the breast tissue often becomes more fatty and less glandular. This can change the texture, size, and overall feel of the breasts.
- Vigilance is Key: Even with these natural changes, it’s crucial to remain alert to any unusual developments, such as lumps, skin changes, or nipple discharge. Any concerns should prompt a visit to a healthcare professional.
Bone Density and Osteoporosis
- The Estrogen Connection: Estrogen plays a vital role in maintaining bone density. As estrogen levels drop post-menopause, many women experience a decrease in bone density, increasing the risk of fractures.
- Osteoporosis: This condition, characterized by weak and brittle bones, becomes a concern for many post-menopausal women. According to the National Osteoporosis Foundation, approximately one in two women over the age of 50 will break a bone due to osteoporosis.
- Bone Density Tests: Women in their 50s and beyond should discuss bone density testing with their doctors. These tests, like the DEXA scan, can assess the risk of osteoporosis and fractures.
In Conclusion
Maintaining optimal breast health is a journey that continues throughout a woman’s life. By staying informed and proactive at every age, you can ensure that you’re doing your best to keep your breasts healthy. Always consult with healthcare professionals about any concerns and remember that early detection is key in addressing potential issues.



